For decades, inhalers were treated as interchangeable tools. A prescription specified the drug, and the device was often secondary. In 2026, that assumption no longer holds. Inhalers have evolved into complex therapeutic systems, where drug, delivery mechanism, usability, and digital integration interact to determine real-world outcomes. This shift reflects a broader change in respiratory care. Clinicians are increasingly aware that pharmacology alone does not guarantee effectiveness. A perfectly selected molecule can fail if delivered incorrectly, inconsistently, or in a way that does not fit the patient’s daily life. At the same time, patients are more informed and more involved in treatment decisions. They compare devices not only on cost, but on how they feel, how easy they are to use, and how well they support long-term disease control.
As a result, the inhaler is no longer just a container for medication. It is an interface between therapy and behavior. Understanding inhaler trends in 2026 means looking beyond price and examining what actually drives outcomes in real use.
Device Design and Ease of Use: The Hidden Driver of Outcomes
The most important differentiator between inhalers in 2026 is not the drug inside, but the device delivering it. Device design directly influences whether medication reaches the lungs effectively, and small differences in usability can translate into large differences in clinical outcomes.
Metered-dose inhalers, dry powder inhalers, and soft mist inhalers each present distinct challenges.
- Metered-dose inhalers require coordination between actuation and inhalation, a task that many patients perform incorrectly even after training.
- Dry powder inhalers depend on sufficient inspiratory flow, which can be difficult for elderly patients or those with severe disease.
- Soft mist inhalers attempt to reduce these barriers by generating a slower, more sustained aerosol, but they introduce their own handling requirements.
Error rates remain high across all device types. Studies have consistently shown that a significant proportion of patients use inhalers incorrectly, leading to reduced drug deposition and suboptimal disease control. In practice, this means that two patients using the same medication may experience very different outcomes depending on their technique.
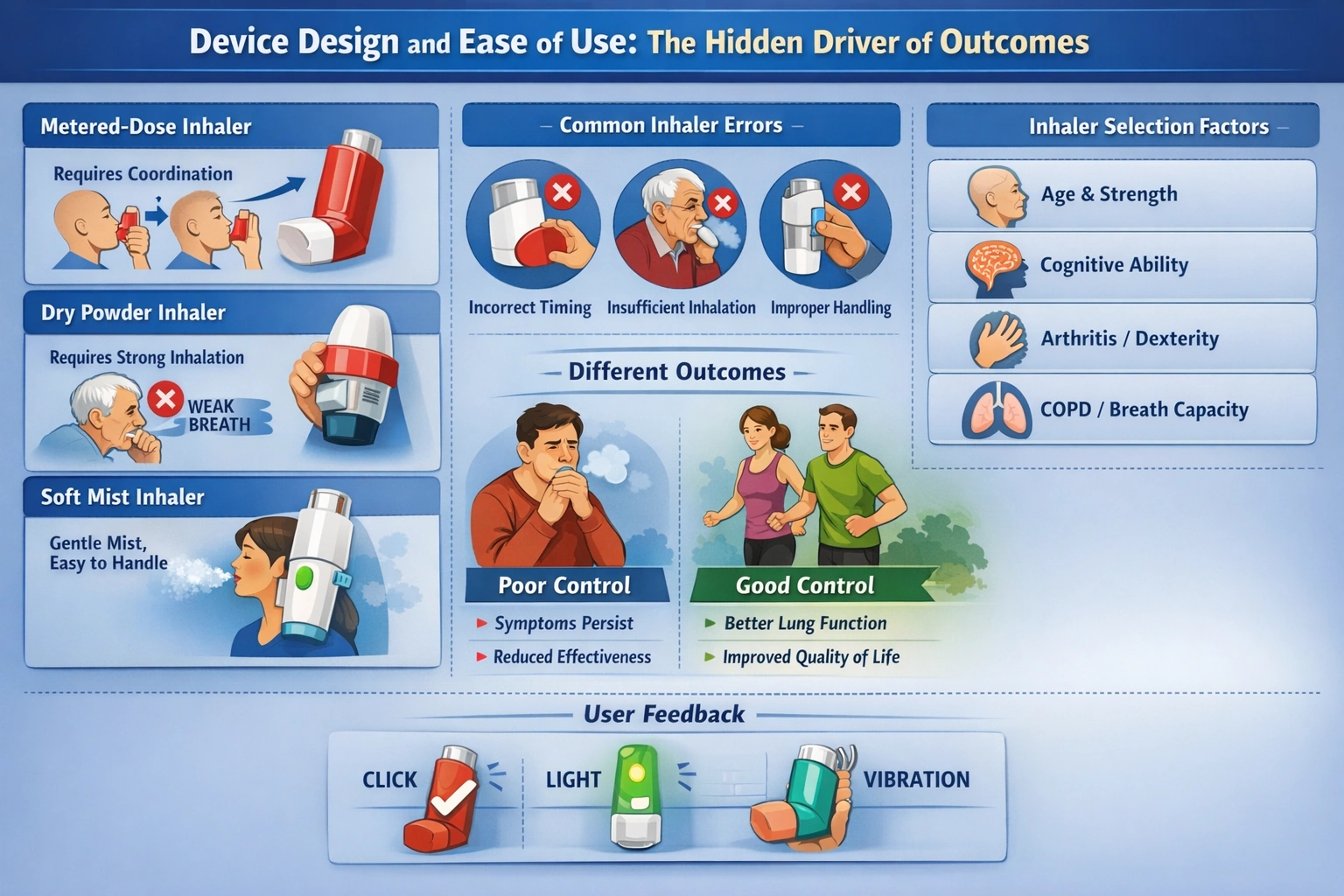 In 2026, clinicians and pharmacists are placing greater emphasis on matching the device to the patient, rather than expecting the patient to adapt to the device. Factors such as age, dexterity, cognitive function, and inspiratory capacity are considered when selecting an inhaler. For example, patients with arthritis may struggle with the force required to actuate certain devices, while those with advanced COPD may not generate sufficient inspiratory flow for dry powder inhalers. Training remains a critical component, but it is no longer seen as sufficient on its own. Even well-trained patients can revert to incorrect technique over time. As a result, there is increasing interest in devices that are inherently easier to use and less prone to error. Design simplicity is becoming a clinical advantage, not just a convenience feature.
In 2026, clinicians and pharmacists are placing greater emphasis on matching the device to the patient, rather than expecting the patient to adapt to the device. Factors such as age, dexterity, cognitive function, and inspiratory capacity are considered when selecting an inhaler. For example, patients with arthritis may struggle with the force required to actuate certain devices, while those with advanced COPD may not generate sufficient inspiratory flow for dry powder inhalers. Training remains a critical component, but it is no longer seen as sufficient on its own. Even well-trained patients can revert to incorrect technique over time. As a result, there is increasing interest in devices that are inherently easier to use and less prone to error. Design simplicity is becoming a clinical advantage, not just a convenience feature.
Another important consideration is feedback. Some newer inhalers provide tactile, auditory, or visual cues that confirm correct use. These features help patients understand whether they have taken a dose properly, reducing uncertainty and improving confidence. In contrast, traditional devices often provide little feedback, leaving patients unsure whether the medication was delivered effectively.
Pharmacies are also adapting to this shift. Pharmacists are spending more time demonstrating device use, correcting technique, and reinforcing proper inhalation patterns. In many cases, device selection is discussed at the point of dispensing, particularly when multiple options are available for the same medication.
Ultimately, the trend is clear. The best inhaler is not the most technologically advanced or the most widely prescribed, but the one the patient can use correctly every time. Device design has moved from the background to the center of therapeutic decision-making.
Drug Formulations and Combination Therapies
While device design determines how medication is delivered, the composition of that medication remains central to treatment strategy. In 2026, one of the most important trends is the continued shift toward combination therapies delivered through a single inhaler.
For both asthma and COPD, combining different classes of drugs in one device has become standard practice. Inhaled corticosteroids, long-acting beta agonists, and long-acting muscarinic antagonists are frequently used together to address multiple aspects of airway disease. This approach simplifies treatment regimens and reduces the need for multiple inhalers, which can improve adherence and reduce confusion. Single-inhaler triple therapy is particularly significant in COPD management. By delivering three medications in one device, these inhalers reduce regimen complexity and ensure that patients receive all components of their prescribed therapy consistently. This is especially important in populations where adherence is already a challenge.
In asthma, the use of combination inhalers has also evolved. Maintenance and reliever therapy strategies, where the same inhaler is used for both daily control and symptom relief, are becoming more common (Albuterol (Ventolin)). This approach aligns treatment with patient behavior, allowing individuals to adjust usage based on symptoms while maintaining anti-inflammatory coverage.
Patients are increasingly aware of these differences. They are not only comparing inhalers based on cost, but also on how many medications are included and how often they need to use them. A single device used once daily may be more attractive than multiple devices used at different times, even if the underlying drugs are similar. There is also a growing focus on onset of action and perceived effectiveness. Some patients prefer inhalers that provide rapid symptom relief, while others prioritize long-term control. These preferences influence satisfaction and adherence, highlighting the importance of aligning treatment with patient expectations.
Formulation stability and consistency are additional considerations. Advances in formulation science have improved the reliability of dose delivery, reducing variability and enhancing confidence in treatment. This is particularly relevant for chronic conditions where patients depend on consistent medication effects over long periods.
In 2026, the trend toward combination therapies reflects a broader goal of simplifying treatment while maximizing effectiveness. By reducing the number of devices and dosing steps, these inhalers aim to bridge the gap between ideal therapy and real-world use.
Digital Inhalers and Adherence Monitoring
The integration of digital technology into inhaler design represents one of the most significant innovations in respiratory care. Smart inhalers equipped with sensors and connectivity features are transforming how adherence is monitored and supported. These devices can record when and how often an inhaler is used, providing objective data on adherence. Some systems also capture information about inhalation technique, offering insights into whether doses are being taken correctly. This data can be transmitted to mobile applications, where patients receive reminders, feedback, and personalized recommendations.
For clinicians, digital inhalers offer a new level of visibility. Instead of relying on patient self-reporting, they can access detailed usage patterns and identify issues such as missed doses or incorrect technique. This enables more targeted interventions and more informed treatment adjustments.
The impact on adherence is significant. Studies have shown that reminder systems and feedback mechanisms can improve consistency of use, particularly in patients who struggle with routine. Digital support turns adherence from a passive expectation into an active process, guided by data and real-time feedback. Telemedicine integration further enhances this effect. Data from smart inhalers can be shared during remote consultations, allowing clinicians to monitor progress and address problems without requiring in-person visits. This is particularly valuable in managing chronic conditions where regular follow-up is essential.
However, digital inhalers also introduce new considerations. Data privacy, cost, and user acceptance are important factors. Not all patients are comfortable with connected devices, and not all healthcare systems are equipped to integrate this data effectively. Despite these challenges, the trend toward digital inhalation therapy is clear. In 2026, inhalers are increasingly data-generating devices, contributing to a more personalized and proactive approach to respiratory care.
Adherence, Lifestyle Fit, and Patient Preference
Adherence has always been a challenge in respiratory care, but in 2026 it is increasingly understood as a function of lifestyle compatibility rather than simple compliance. Patients are not just following instructions. They are integrating treatment into their daily routines, and the success of that integration depends on how well the inhaler fits their lives.
Frequency of dosing is a key factor. Once-daily inhalers are generally associated with better adherence than those requiring multiple daily doses. Simplicity reduces the likelihood of missed doses and makes treatment easier to maintain over time.
Portability and discreteness also matter. Patients may prefer inhalers that are compact and easy to carry, particularly if they need to use them in public settings. Devices that draw attention or require complex preparation can create barriers to consistent use.
Psychological factors are equally important. Some patients feel stigmatized by visible medication use, while others may associate inhaler use with illness in a way that affects their willingness to adhere. These perceptions can influence behavior in ways that are not captured by clinical metrics. Routine compatibility is another consideration. Patients with structured daily schedules may find it easier to adhere to fixed dosing times, while those with variable routines may benefit from more flexible treatment approaches. The alignment between treatment and daily life is a strong predictor of long-term success.
Education and support play a role, but they are not sufficient on their own. Even well-informed patients may struggle with adherence if the treatment does not fit their lifestyle. This has led to a greater emphasis on shared decision-making, where patients are involved in selecting inhalers that align with their preferences and circumstances.
Environmental Impact and Sustainability Pressures
Environmental considerations are becoming an increasingly visible factor in inhaler selection. Traditional metered-dose inhalers use propellants with a significant carbon footprint, while dry powder inhalers have a lower environmental impact. This difference is attracting attention from regulators, healthcare systems, and patients.
In some regions, particularly in Europe, there is growing pressure to reduce the environmental impact of inhaler use. Guidelines and policy initiatives are encouraging the adoption of lower-emission devices where clinically appropriate. This is influencing prescribing patterns and raising awareness among patients. Patients themselves are also becoming more conscious of sustainability. For some, the environmental impact of their medication is an important consideration, particularly when multiple therapeutic options are available. While this factor does not yet dominate decision-making, it is gaining relevance.
Pharmacies are beginning to engage with this trend by providing information about environmental differences and, in some cases, offering recycling programs for inhaler components.
Conclusion
The inhaler landscape in 2026 reflects a broader shift in healthcare. Price remains important, but it is no longer the dominant factor in decision-making. Patients and clinicians are increasingly focused on real-world performance, where usability, adherence, and therapeutic design determine outcomes.
Device design influences whether medication is delivered effectively. Combination therapies simplify regimens and improve consistency. Digital technologies support adherence and enable more personalized care. Lifestyle fit determines whether patients can sustain treatment over time. Environmental considerations add a new dimension to decision-making. Taken together, these factors redefine what it means to choose an inhaler. It is no longer about selecting a product, but about selecting a system that works in practice.
As inhalers continue to evolve, the distinction between device and therapy will become less clear. They are becoming integrated platforms that combine pharmacology, technology, and user experience. In this context, the most important question is not which inhaler is cheapest, but which one delivers the best outcomes in the realities of everyday life.